>> Researchers Identify a Key Immune Pathway in Fungal Gut Colonization
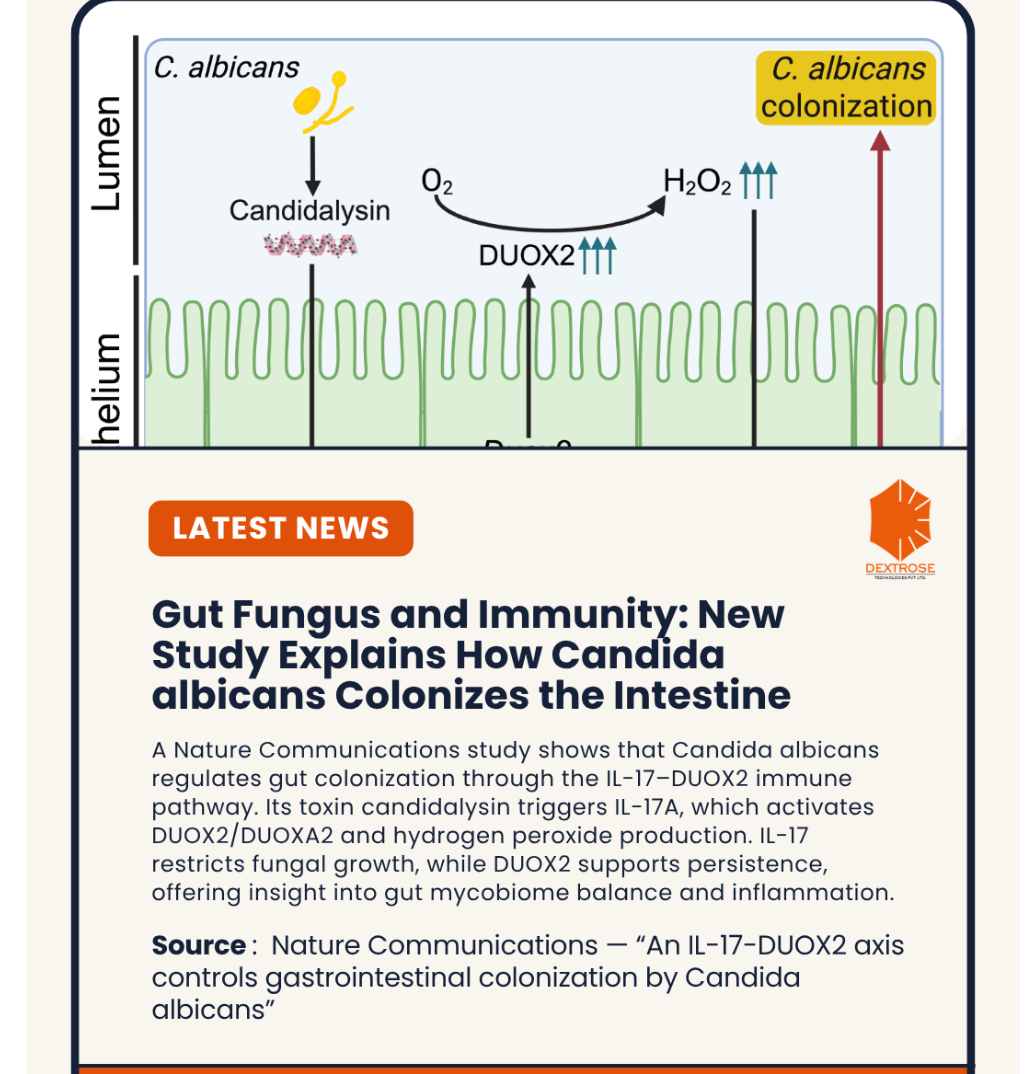
A new study published in Nature Communications has revealed how the common gut fungus Candida albicans interacts with the host immune system to regulate its colonization in the gastrointestinal tract. The study identifies an important immune pathway called the IL-17–DUOX2 axis, which helps control how the fungus persists in the gut.
>> Why Candida albicans Matters
Candida albicans is a fungus commonly found in the human gut. In most people, it exists harmlessly as part of the gut microbiome. However, under certain conditions, such as immune imbalance, antibiotic use, or gut dysbiosis, it can overgrow and contribute to infection or inflammation.
The study highlights that C. albicans is not just a passive organism in the gut. Instead, it actively communicates with host immune and epithelial cells, influencing both fungal survival and host defense responses.
>> Focus on the Ileum and Colon
The researchers studied how C. albicans colonization affects gene expression in the intestine. They found strong changes in the ileum and colon, two important regions of the gastrointestinal tract.
A major finding was the increased expression of two genes: DUOX2 and DUOXA2. These genes are involved in producing hydrogen peroxide, a molecule that helps the body respond to microbes in the gut.
>> Role of the IL-17 Immune Signal
The study found that the immune molecule IL-17A plays a central role in activating DUOX2 and DUOXA2. IL-17A is an inflammatory cytokine involved in mucosal immunity and defense against fungal organisms.
When IL-17 signaling was reduced, C. albicans colonization increased. This suggests that IL-17 helps limit fungal growth in the intestine.
>> Candidalysin Triggers the Host Response
A key fungal factor identified in the study is candidalysin, a toxin produced by the hyphal form of C. albicans. Hyphae are filament-like fungal structures often associated with stronger host responses.
The researchers found that candidalysin helps stimulate IL-17A production. This then activates the DUOX2 pathway in intestinal epithelial cells, showing a direct link between fungal morphology, toxin production, and host immune signaling.
>> DUOX2 Has a Complex Role
DUOX2 is generally associated with antimicrobial defense because it supports hydrogen peroxide production. However, the study found that DUOX2 also influences fungal persistence in the gut.
While IL-17 signaling restricted C. albicans colonization, DUOX2 activity appeared to support fungal colonization under certain conditions. This shows that the immune response is not simply “anti-fungal” but is part of a more balanced interaction between host and microbe.
>> Findings from Mouse and Colonoid Models
The research used germ-free mice, antibiotic-treated mice, IL-17 receptor-deficient mice, DUOX2-deficient models, and intestinal colonoids. These models helped show that C. albicans induces DUOX2-related responses through IL-17 signaling and candidalysin activity.
In colonoid experiments, IL-17A stimulation increased DUOX2 and DUOXA2 expression and promoted hydrogen peroxide production. This confirmed that intestinal epithelial cells can directly respond to IL-17A through the DUOX2 pathway.
>> Link to Gut Inflammation
The study notes that DUOX2 and DUOXA2 have been linked to intestinal homeostasis and inflammatory bowel disease. Since C. albicans is also associated with inflammatory bowel conditions, these findings may help researchers better understand how fungal organisms contribute to gut inflammation.
>> Why This Study Is Important
This research provides new insight into how fungi and the immune system interact inside the gut. It shows that C. albicans colonization is regulated by a complex relationship involving fungal toxin production, IL-17 immune signaling, epithelial DUOX2 activity, and hydrogen peroxide production.
>> Key Takeaway
The study demonstrates that Candida albicans uses its hyphal toxin candidalysin to activate IL-17 responses, which in turn stimulate DUOX2 activity in the gut epithelium. This immune pathway helps regulate fungal colonization and may offer new clues for understanding fungal involvement in intestinal diseases.